Lunchtime pandemic reading.
Standard disclaimer: this is a roundup of informative pieces I've read that interest me on the severity of the crisis and how to manage it. I am not a qualified medical expert in ANY sense; at best I am reasonably well-read laity. ALWAYS prioritize advice from qualified healthcare experts over some person on Facebook.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.
You are welcome to share this.
---
My parents asked me last night what our travel plans were for the holidays (they live about 5 hours away by car), and I said as kindly as I could that we have none - and neither should they. We are heading into the holiday season with as many cases brewing as we did at the peak of summer here in the United States, and I don't want my family getting sick. My parents are in the highest-risk group by age; you know what I do want for the holidays? A funeral right after, no matter how much I might miss seeing them.
Be prepared to have that difficult conversation with your relatives and friends. While we may be able to tamp down our levels of infections, chances are it will be a difficult struggle for many nations. Keep yourself and your loved ones safe. Stay home if you can this holiday season.
---
You know things are getting serious when New England stops ice hockey. "All indoor ice rinks and ice skating facilities in Massachusetts are prohibited from operating for the next two weeks due to rising coronavirus cases connected to indoor ice hockey, the state's Department of Public Health announced Thursday night.
Officials say the new public health order is in response to multiple COVID-19 clusters occurring at rinks throughout the state following games, practices and tournaments. Nearly 110 cases of the virus have been directly connected to hockey, the DPH said in a press release.
Health officials say this two-week pause will allow stronger COVID-19 protocols to be developed to further protect players, families, coaches, arena staff and other participants, as well as communities surrounding hockey rinks.
Current protocols include limits on the number of people allowed in an arena and social distancing."
Source: https://www.nbcboston.com/news/coronavirus/mass-pausing-indoor-ice-hockey-for-2-weeks-due-to-increasing-covid-19-cases/2216708/
Commentary: We saw this coming. There's an ice hockey rink near my house and people are simply not following protocols. They're congregating without masks in the parking lot close together. They're arriving with their kids not suited up to play (regulations say no use of the changing areas at all). They're wearing masks incorrectly or not at all.
Disease does not respect your social status. It does not respect how special you feel you or your children are. It does not respect beliefs. Disease does what disease does, and it only needs a few minutes to infect you. There's no forgiveness for lapses. There's no excusing yourself.
The only way through for all of us is constant vigilance and continued adherence - without exception - to protocols to protect ourselves and others.
---
Tocilizumab (monoclonal antibody) shows no effect. "We performed a randomized, double-blind, placebo-controlled trial involving patients with confirmed severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, hyperinflammatory states, and at least two of the following signs: fever (body temperature >38°C), pulmonary infiltrates, or the need for supplemental oxygen in order to maintain an oxygen saturation greater than 92%. Patients were randomly assigned in a 2:1 ratio to receive standard care plus a single dose of either tocilizumab (8 mg per kilogram of body weight) or placebo. The primary outcome was intubation or death, assessed in a time-to-event analysis. The secondary efficacy outcomes were clinical worsening and discontinuation of supplemental oxygen among patients who had been receiving it at baseline, both assessed in time-to-event analyses.
Tocilizumab was not effective for preventing intubation or death in moderately ill hospitalized patients with Covid-19. Some benefit or harm cannot be ruled out, however, because the confidence intervals for efficacy comparisons were wide. (Funded by Genentech; ClinicalTrials.gov number, NCT04356937"
Source: https://www.nejm.org/doi/full/10.1056/NEJMoa2028836
Commentary: Monoclonal antibodies have been in the headlines for quite some time, especially with the United States president receiving a compassionate use exemption for it, despite it not having passed clinical trials. As we're now seeing, some of these solutions may not have any benefit.
---
How fast do we see changes in cases with non-pharmaceutical interventions? "To the best of our knowledge, this study is the first to explicitly quantify the effects of both introducing and lifting individual NPIs on R over time. By linking a global dataset of country-level daily R values with a global dataset of country-level policies on NPIs, we modelled the change in R values (as R ratio) from day 1 to day 28 following the introduction and relaxation of eight individual NPIs among 131 countries. We found that reopening schools, lifting bans on public events, lifting bans on public gatherings of more than ten people, lifting requirements to stay at home, and lifting internal movement limits were associated with an increase in R of 11–25% on day 28 following the relaxation. However, the effects of introducing and lifting NPIs were not immediate; it took a median of 8 days (IQR 6–9) following the introduction of NPIs to observe 60% of their maximum reduction in R and even longer (17 days [14–20]) following the relaxation to observe 60% of the maximum increase in R. A similar delay in response to the introduction and relaxation of NPIs was also identified using Google mobility data. We compared four different candidates of composite NPIs that countries might consider in response to a possible resurgence of COVID-19.
We quantified the change in transmission of SARS-CoV-2, as measured by R, following the introduction and relaxation of individual NPIs, and found a delay of 1–3 weeks in observing the effects of introducing and lifting these NPIs. These findings provide additional evidence that can inform policy-maker decisions on which NPIs to introduce or lift and when to expect a notable effect following the introduction or the relaxation."
Source: https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(20)30785-4/fulltext
Commentary: This is a really important piece because that 1-3 week delay is critical for understanding cases and the news cycle. What you're seeing when you look at data about cases is a snapshot of how things were 1-3 weeks ago, in a sense - any changes you make today won't be reflected for 1-3 weeks.
So if, as we see in the hockey story above, a government changes policy and allows for a 2-week period, that may not be enough time to judge whether something is working. Better to wait at least 3 weeks.
If you want to play it safe personally, when a government announces the lifting of a restriction, continue to act as though the restriction were in place for 3 weeks and see what happens with case counts.
---
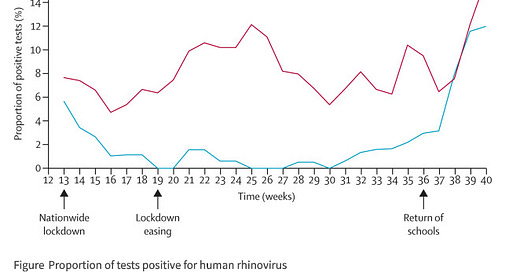
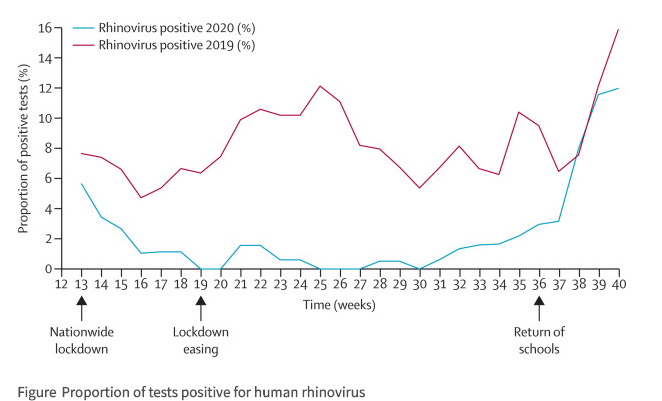
Lockdowns and the common cold. "In the past few weeks, there has been a great deal of trepidation among the public about the impact of children returning to school on the transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Children have greater difficulty adhering to physical distancing rules but are believed to transmit the virus less efficiently than adults.1 Rhinoviruses normally circulate year-round with seasonal peaks in spring and autumn and are transmitted in largely the same manner as SARS-CoV-2. Children are the main drivers of transmission of rhinovirus, with subsequent transmission to adults associated with exacerbations of airways disease and hospitalisations.2
Our data support previous reports that children are a major reservoir for rhinovirus infection, and a key driver of transmission to adults. Furthermore, our data suggests that current physical distancing measures adopted by schools do not effectively prevent rhinovirus transmission. These findings might have important implications for circulation of both influenza and SARS-CoV-2 in the coming winter months. If current distancing measures in schools do not prevent rhinovirus transmission, it seems likely that the same will hold true for influenza, for which young children are also known to be key transmitters.5 The implications for SARS-CoV-2 are less clear, as young children appear to be less susceptible to infection than older children or adults, but once infected they have similar levels of detectable virus in the nasopharynx.6"
Source: https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30502-6/fulltext
Commentary: This is a wonderful and obvious visualization. Once schools opened up, the common cold surged back into action. It's a respiratory disease, so is anyone surprised when schools are seeing COVID-19 spikes? They shouldn't be. Kids are disease carriers par excellence - they are in close proximity, have relatively poor hygiene, and are unlikely to stringently adhere to protocols for disease mitigation. It's one of the reasons why we have so many vaccines administered to kids - because they're massive spreaders.
---
We don't know what happens if you catch COVID-19 and the flu at the same time. "Influenza is notoriously difficult to predict. In terms of how a large outbreak would affect the COVID-19 pandemic, there is not that much that can be said with certainty. “We know very little about co-infection or the interaction between SARS-CoV-2 and influenza”, points out Salmon. “There just have not been enough cases for us to draw any conclusions.” Crucial unanswered questions include: how does co-infection with SARS-CoV-2 and influenza affect mortality from either disease? Is a patient infected with one virus more likely to contract the other? Is the influenza vaccine protective against SARS-CoV-2?
Clinicians will have to become accustomed to distinguishing between influenza and COVID-19. The similar symptoms makes this something of a challenge. “Diagnostics for flu are widely available, but we really need a rapid test for SARS-CoV-2; something sensitive and specific, with a high positive predictive value”, Salmon told The Lancet Respiratory Medicine. “This is not a situation where we should be making diagnoses based on clinical signs alone.” Misdiagnosis could lead to all kinds of problems. Influenza and COVID-19 have different recommended treatments and patients with influenza are not typically told to isolate. “We also need to bear in mind that a diagnosis of COVID-19 or influenza alone would be insufficient to exclude the presence of another co-infecting pathogen”, adds Benjamin Singer, assistant professor of medicine (Pulmonary and Critical Care) at Northwestern University (Chicago, Illinois, USA).
Amid all the uncertainty, experts are agreed on one matter. “We really need to ramp up vaccination against influenza”, said Singer. The UK has ordered 30 000 doses of the influenza vaccine. It aims to vaccinate a wide range of groups, including the older population, health and social care workers, children aged 2–3 years, as well as those in year 7 of school. “The influenza vaccine is by no means perfect”, concluded Singer. “But if countries manage to get as many people vaccinated as possible, they would put themselves in the best possible position to minimise the burden on health-care systems.”"
Source: https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30508-7/fulltext
Commentary: The Southern Hemisphere largely did a great job controlling COVID-19 with stringent lockdowns. AS a result, they saw basically no flu season. Whether the Northern Hemisphere follows suit remains to be seen, but the good news is that the same precautions we take for COVID-19 also work against influenza - and there's a vaccine for the flu. Get it if you can, and stringently adhere to COVID-19 prevention protocols. If you do, there's a good chance you won't get sick from a respiratory disease at all this winter in the Northen Hemisphere.
---
A reminder of the simple daily habits we should all be taking.
1. Wash/sanitize your hands every time you are in or out of your home for any reason. Consider also spraying the bottoms of your shoes with a general disinfectant (alcohol/bleach/peroxide) when you return home. Remember that cleaners are NEVER to be ingested or injected.
2. Always wear a mask when out of your home and if going to a high risk area, wear goggles. Respirators are back in stock at online retailers, too.
3. Stay home as much as possible. Minimize your contact with others and maintain physical distance of at LEAST 6 feet / 2 meters, preferably more. Avoid indoor places as much as you can; indoor spaces spread the disease through aerosols and distance is less effective at mitigating your risks.
4. Get your personal finances in order now. Cut all unnecessary costs.
5. Replenish your supplies as you use them. Avoid reducing your stores to pre-pandemic levels in case an outbreak causes unexpected supply chain disruptions.
6. Participate in your local political process. For Americans, go to Vote.org and register/verify your vote.
7. Ventilate your home as frequently as weather and circumstances permit.
---
Common misinformation debunked!
There is no genomic evidence at all that COVID-19 arrived before 2020 in the United States and therefore no hidden herd immunity:
Source:

There is no evidence SARS-CoV-2 was engineered, nor that it escaped a lab somewhere.
Source: https://www.washingtonpost.com/world/2020/01/29/experts-debunk-fringe-theory-linking-chinas-coronavirus-weapons-research/
Source: https://www.nature.com/articles/s41591-020-0820-9
Source: https://www.nationalgeographic.com/science/2020/05/anthony-fauci-no-scientific-evidence-the-coronavirus-was-made-in-a-chinese-lab-cvd/
There is no evidence a flu shot increases your COVID-19 risk.
Source: https://www.factcheck.org/2020/04/no-evidence-that-flu-shot-increases-risk-of-covid-19/
Source: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa626/5842161
---
A common request I'm asked is who I follow. Here's a public Twitter list of many of the sources I read.
https://twitter.com/i/lists/1260956929205112834
This list is biased by design. It is limited to authors who predominantly post in the English language. It is heavily biased towards individual researchers and away from institutions. It is biased towards those who publish or share research, data, papers, etc. I have made an attempt to follow researchers from different countries, and also to make the list reasonably gender-balanced, because multiple, diverse perspectives on research data are essential.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.