Lunchtime pandemic reading.
Standard disclaimer: this is a roundup of informative pieces I've read that interest me on the severity of the crisis and how to manage it. I am not a qualified medical expert in ANY sense; at best I am reasonably well-read laity. ALWAYS prioritize advice from qualified healthcare experts over some person on Facebook.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.
You are welcome to share this.
--
As of today, we have hit some milestones. 31 million people planetwide with known cases since the start. 961,544 deaths worldwide directly attributed. In the United States, one-fifth of those deaths as we cross the 200,000 dead milestone.
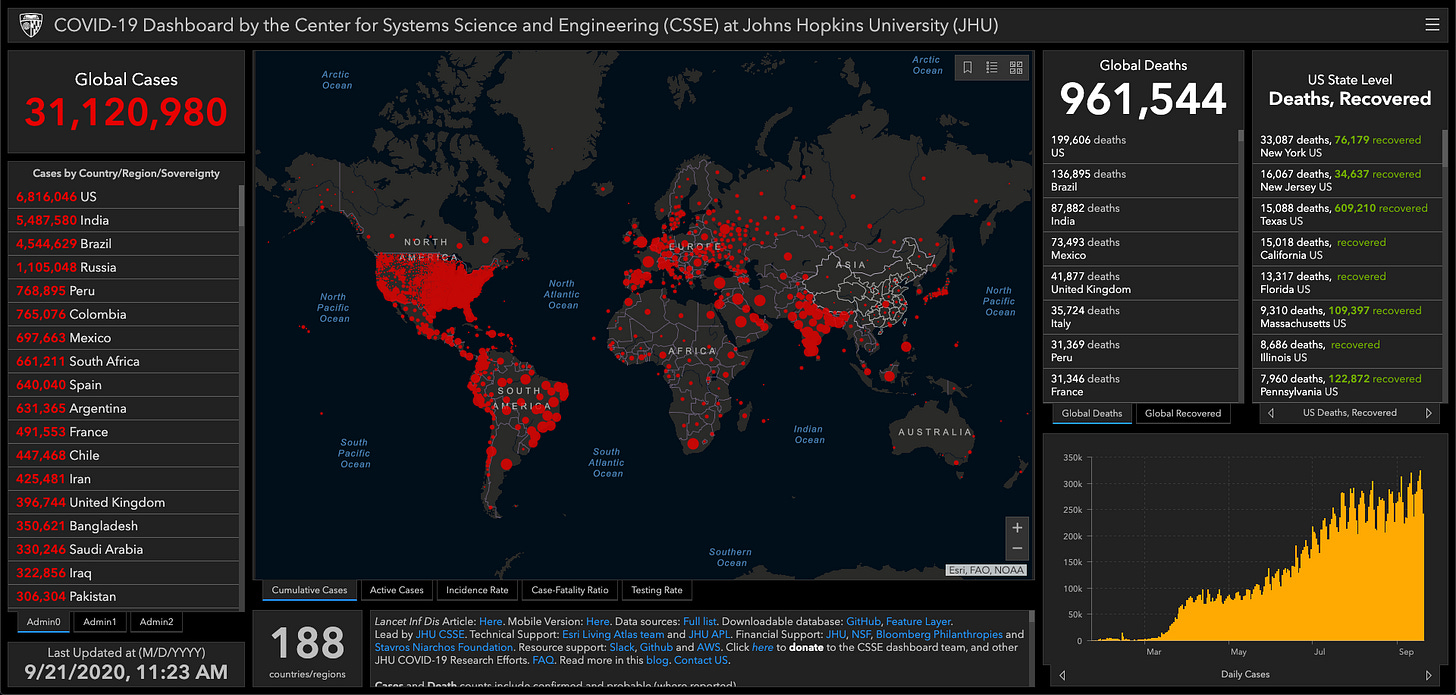
As Mother Jones said, "Pray for the dead. Fight like hell for the living." We are heading into dangerous territory in the Northern Hemisphere and cases are rising in many geographies.
Stay vigilant. Wear a mask out of your home. Watch your distance around others. Wash/sanitize your hands every time you're out of your home and returning home. Don't touch your face for any reason until you've sanitized your hands. Stay out of indoor spaces that aren't your home as much as practical.
That said, DO continue to enjoy the outdoors (away from people) as much as you can while the weather is nice. DO continue to reach out, chat with friends, start new hobbies, get involved in your community, and all the other behaviors that pose low risk but give you that sense of connection to others.
We in the Northern Hemisphere have a long road ahead of us, the next 6 months. Build your plan now for how you're going to handle it.
--
FRom the talk show circuit, Dr. Scott Gottlieb: "Well, I think we have at least one more cycle with this virus heading into the fall and winter. If you look what's happening around the country, right now, there's an unmistakable spike in new infections. And you're also seeing declines in hospitalizations that we were achieving starting to level off, I would expect them to start going up again, as well. There's about 15 states with a positivity rate is 10% or higher, which is deeply concerning. There's about 30 states where the RT the rate of transfer is above one, meaning they have an expanding epidemic. So right now we're seeing a resurgence of infection. Now, whether or not that's a post Labor Day bump and will start to level off, or this is the beginning of a resurgence heading into the fall in the winter. It's unclear, but I'm deeply concerned that as we head into the fall in the winter, this is the season when a respiratory pathogen like Coronavirus, wants to spread. And so there's a lot of risk heading into this season.
Well, right now we're seeing infections go up around the country, the Northeast still is holding on to the gains that it achieved and driving down infections, but we're seeing infections starting to rise in the south as well. And you're definitely seeing a concentration of new infections in the Midwest. That's that's driving a lot of the growth and infections. But it's getting more distributed around the country. And the concern is that as we get a little bit more complacent, because we are exhausted as a population from what we've been going through, we head back to school and college people try to go back to work against the backdrop of the fall in the winter when people are heading indoors. Because the weather's cooling. That's a real setup for risk. And there hasn't been enough people exposed to this virus at this point across the country that we have enough background immunity, that that's going to really stop the rate of transfer. I mean, it may slow it in certain parts of the country. It's been epidemic like Miami or Houston or New York, but most parts of the country is still vulnerable. And in fact, when you look at what's happening in Arizona right now, you're starting to see cases go back up even there and that place was very hard hit. And so it's an indication that there's a lot of virus left to go in this country."
Source:
Commentary: We're already not testing enough in the United States. To see 10% positivity rates is really a problem going into the fall and winter because we need to know what we're going up against.
Could you imagine starting a game of 5-card draw poker but you can't see 2 of your 5 cards? That's an analogy to how poorly we're testing in America.
--
Dr. Nahid Bedelia: "And, you know, just to stress the 200,000 that we're seeing, those are deaths. I think when we look back on this retrospect of a lens, that we're sort of getting a fuller picture, we'll look at the people who carry the burden of hospitalizations that people carry the burden of having long COVID, you know, the debilitating symptoms that we're seeing at least 10% of these patients who have COVID-19."
Source:
Commentary: This is the first time I've heard a hard number around the long-term consequences of COVID-19 in a while. Early on, it was stated that 5% of the cases would be severe, but we didn't (and couldn't) know the long-term number. 10% of people who contract COVID-19 having serious, long-term complications is a BIG number. Consider that for a moment. 3.1 million people around the world then have long-term, possibly life-long illness or disability.
That also frames the debate more easily about things like masks. A 1% fatality rate seems like a small number (even though it's not). But a 10% chance of lifelong disability? Those are terrible odds, odds people can understand.
--
More on transmission dynamics.
"The risk of transmission is complex and multi-dimensional. It depends on many factors: contact pattern (duration, proximity, activity), individual factors, environment (i.e. outdoor, indoor) & socioeconomic factors (i.e. crowded housing, job insecurity). (2/n)
We now know that sustained close contact drives the majority of infections and clusters. For instance, close family/friend contacts and gatherings are a higher risk for transmission than market shopping or brief community encounters. (3/n)
Even in the same household being a spouse/partner, sleeping in the same room or sharing the same sleeping space, frequent daily contact with the index case, and dining in close proximity has been associated with increased risk of transmission. (4/n)
For non-household contacts, engaging in group activities such as dining together or board games have been found to be high risk for transmission. So, the risk increases with longer & frequent exposure, close proximiZty, # of contacts, and group activities especially dining (5/n)
Many ppl either do not infect anyone or infect a single person, and a large number of secondary cases are caused by a small # of infected ppl. Although this also is related to other factors, individual variation in infectiousness plays a major role.(6/n)
When we look at the viral load dynamics & contact tracing studies, those who are infected are very infectious for a short window, likely 1-2 days before and 5 days following symptom onset. No transmission documented so far after the first week of symptom onset. (7/n)
While asymptomatic patients can transmit the virus to others, emerging evidence suggests that asymptomatic index cases transmit to fewer secondary cases. Attack rates are highly correlated with symptom severity (8/n)
Contact pattern also depends on the setting of the encounter. Contact tracing studies suggest an almost 20x higher risk of transmission indoors compared with outdoor environments. (10/n) (https://ft.com/content/2418ff87-1d41-41b5-b638-38f5164a2e94)
Prolonged indoor contact in a crowded and poorly ventilated environment increases the risk of transmission substantially. But decreasing occupancy and improving ventilation through opening windows/doors can lower the risk. (11/n)"
Source:


Source: https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3692807
Commentary: 7 months in, we're still trying to figure out how this bug works; we're closer to explanations now than we used to be, but let's be honest: there's still so much we don't know.
--
I'd never heard of the NMA until today. Now I know, and now you do, too. "s trust in federal health agencies has withered over the last few months, a group of Black physicians has been working on an antidote: creating their own expert task force to independently vet regulators’ decisions about Covid-19 drugs and vaccines as well as government recommendations for curbing the pandemic.
Organized by the National Medical Association — founded in 1895 as an answer to racist professional societies excluding Black doctors — the committee is meant to safeguard against any unscientific guidance from the Centers for Disease Control and Prevention and the Food and Drug Administration.
“It’s necessary to provide a trusted messenger of vetted information to the African American community,” said Leon McDougle, a family physician and president of the NMA. “There is a concern that some of the recent decisions by the Food and Drug Administration have been unduly influenced by politicians.”
McDougle frames the new task force as a way to address the suspicion that has sprouted up around Covid-19 vaccines. Some worry that, in being developed at “warp speed,” the shots might not be safe or properly tested before they’re approved, and the anxiety is only heightened for those who’ve been alienated by the medical system. That’s part of the reason that certain patients of color are especially wary of taking part in the clinical trials — and those concerns may well persist even if adequate studies are done and a vaccine hits the market.
“I think this will help to increase uptake in the African American community, if members of our task force give it the green light,” McDougle said. But he emphasized that their stamp of approval would come only if data show that the vaccine is, in fact, effective and safe.
They’ll also be evaluating how well the clinical trial participants represent the demographic breakdown of the American population, as well as the fairness of the federal plans to distribute a vaccine — both of which are especially important given the disproportionate impact that the pandemic has had on Black, Latino, and Native American communities.
“There is a need for this task force. We need a trusted organization to take the lead on this effort,” said emergency physician Uché Blackstock, the founder and CEO of the consulting firm Advancing Health Equity, who is not a member of the NMA. “What we’ve seen in terms of political interference in the FDA and CDC has really undermined what little trust the Black community had.”"
Source: https://www.statnews.com/2020/09/21/black-doctors-group-creates-panel-to-vet-covid19-vaccines/
Commentary: This is a terrific initiative. The more credible experts who are examining all the data around vaccines, the better. If the leading experts all look at the clinical trials data and say yes, it's working, it's safe, etc. then we can trust in whatever vaccines they approve. I think having a foil to the official government agencies, especially when there's strong evidence of political interference (see https://www.nytimes.com/2020/09/19/health/azar-hhs-fda.html for more) is essential.
--
A reminder of the simple daily habits we should all be taking.
1. Wash/sanitize your hands every time you are in or out of your home for any reason. Consider also spraying the bottoms of your shoes with a general disinfectant (alcohol/bleach/peroxide) when you return home. Remember that cleaners are NEVER to be ingested or injected.
2. Always wear a mask when out of your home and if going to a high risk area, wear goggles. Respirators are back in stock at online retailers, too.
3. Stay home as much as possible. Minimize your contact with others and maintain physical distance of at LEAST 6 feet / 2 meters, preferably more. Avoid indoor places as much as you can; indoor spaces spread the disease through aerosols and distance is less effective at mitigating your risks.
4. Get your personal finances in order now. Cut all unnecessary costs.
5. Replenish your supplies as you use them. Avoid reducing your stores to pre-pandemic levels in case an outbreak causes unexpected supply chain disruptions.
--
Common misinformation debunked!
There is no genomic evidence at all that COVID-19 arrived before 2020 in the United States and therefore no hidden herd immunity:
Source:

There is no evidence SARS-CoV-2 was engineered, nor that it escaped a lab somewhere.
Source: https://www.washingtonpost.com/world/2020/01/29/experts-debunk-fringe-theory-linking-chinas-coronavirus-weapons-research/
Source: https://www.nature.com/articles/s41591-020-0820-9
Source: https://www.nationalgeographic.com/science/2020/05/anthony-fauci-no-scientific-evidence-the-coronavirus-was-made-in-a-chinese-lab-cvd/
There is no evidence a flu shot increases your COVID-19 risk.
Source: https://www.factcheck.org/2020/04/no-evidence-that-flu-shot-increases-risk-of-covid-19/
Source: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa626/5842161
--
A common request I'm asked is who I follow. Here's a public Twitter list of many of the sources I read.
https://twitter.com/i/lists/1260956929205112834
This list is biased by design. It is limited to authors who predominantly post in the English language. It is heavily biased towards individual researchers and away from institutions. It is biased towards those who publish or share research, data, papers, etc. I have made an attempt to follow researchers from different countries, and also to make the list reasonably gender-balanced, because multiple, diverse perspectives on research data are essential.



