Lunchtime pandemic reading.
Standard disclaimer: this is a roundup of informative pieces I've read that interest me on the severity of the crisis and how to manage it. I am not a qualified medical expert in ANY sense; at best I am reasonably well-read laity. ALWAYS prioritize advice from qualified healthcare experts over some person on Facebook.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.
You are welcome to share this.
---
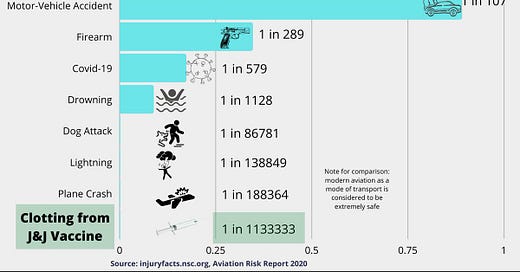
A retraction - the J&J vaccine isn't 1,000 times safer than the car you're driving in, it's 10,000 times safer.
Source:


Commentary: Of even greater importance is the likelihood of getting the same blood clotting issues from COVID-19: 2,000 times more likely. Get the vaccine. Get ANY vaccine. They work, and they're safe.
---
Leave the middle seat open. "Based on laboratory modeling of exposure to SARS-CoV-2 on single-aisle and twin-aisle aircraft, exposures in scenarios in which the middle seat was vacant were reduced by 23% to 57%, compared with full aircraft occupancy, depending upon the model.
Physical distancing of airplane passengers, including through policies such as middle seat vacancy, could provide additional reductions in risk for exposure to SARS-CoV-2 on aircraft."
Source: https://www.cdc.gov/mmwr/volumes/70/wr/mm7016e1.htm?s_cid=mm7016e1_w
Commentary: It's nice to put a number to a common sense qualitative concept. Of course, sitting closer to someone increases risk of infection - and not just for COVID-19, but for anything your fellow traveler may be carrying that's airborne like the flu and the common cold. Even after the pandemic is over, my days of traveling without a mask will be long gone in the before times. Mask up for traveling and stay healthy.
---
The cupboard is still relatively bare. "Aside from one qualified success in remdesivir, a therapy originally developed to treat hepatitis C and Ebola, there were practically no strong antiviral drug candidates to quickly test and deploy against SARS-CoV-2. Researchers bemoan that there weren’t more options. “We need an arsenal,” says Kara Carter, head of discovery biology at the biotech company Dewpoint Therapeutics in Boston, Massachusetts, and president of the International Society for Antiviral Research.
New initiatives to create that arsenal are on the horizon. The US National Institutes of Health (NIH), for one, is planning a major programme to develop therapeutics against SARS-CoV-2 variants and other viruses with pandemic potential. A new industry-backed coalition is taking aim at influenza viruses and coronaviruses. And a few groups hope to create antivirals for more distantly related pathogens that pose a pandemic risk.
Because viruses in general are poor at catching genetic mistakes, these types of therapy — called nucleoside analogues — often work across viral families. Antiviral drugs that bind enzymes directly and block their function — which is to say, the vast majority of antivirals — do not typically have such broad activity. In principle, scientists could design drugs that work in many viruses by going after the most highly conserved regions of target proteins, says Jasper Fuk-Woo Chan, an emerging infectious-disease researcher at the University of Hong Kong. But, he adds, “traditionally, it’s always been a ‘one bug, one drug’ approach”.
In many ways, the narrow activity of existing antivirals boils down to the nature of viruses themselves. Other types of pathogen — bacteria, fungi, parasites — are more easily contained because their cellular properties offer an abundance of targets for drug activity. Think about penicillin, which blocks cell-wall synthesis. Or azole antifungals, which disrupt the cell membrane.
Viruses, with their compact genomes and lack of cellular anatomy, offer many fewer druggable targets. Add in a high rate of replication — a typical SARS-CoV-2 infection, for instance, is thought to produce more than one million virions per person per day6 — coupled with an inherent genetic mutability, and it’s no wonder that most existing antivirals proved useless for COVID-19.
The plasticity of viruses means that a drug with activity against, say, herpes is unlikely to make a dent against a coronavirus. Alejandro Chavez, a bioengineer and antiviral drug researcher at Columbia University Irving Medical Center in New York City, thus doubts that anyone will find a “godly inhibitor that’s basically going to block everything”.
“What we will hopefully find”, he says, “are inhibitors that work on, if you’re really lucky, an entire family.” That would make the best-case scenario a pan-coronavirus inhibitor. But a more reasonable goal might be developing a drug for a subset of coronaviruses, such as alphacoronaviruses, which currently cause non-lethal infections in humans, and having a different drug for betacoronaviruses, the group responsible for SARS, MERS, and COVID-19."
Source: https://www.nature.com/articles/d41586-021-00958-4
Commentary: This was a fascinating read, and emphasizes that we, as a species, need to invest more in R&D to prevent and mitigate the damage done by disease. The good news is we're not starting from scratch, but what each of us can do is lobby our elected officials to keep investing in R&D as a public good.
---
India's seeing the double spike mutation. "Double mutation has been detected in 61 per cent of the total 361 Covid-19 samples tested between January and March this year, a genome sequencing expert claimed on Wednesday even as he raised doubts over the methods of sample collection being adopted by authorities in Maharashtra, which is worst affected by the pandemic.
However, experts in the fields of genome sequencing and cell science have observed that such a small sample size cannot be considered as an indication of the spread of the mutated virus.
These 361 samples were tested at the genome sequencing laboratories in Maharashtra.
On the other hand, authorities and officials of civic bodies that are collecting Covid-19 samples daily have complained about the lack of communication from the genome sequencing laboratories in Maharashtra as well as from the Centre about their findings on the sample analysis.
This lack of communication is resulting in civic bodies and state health officials remaining in the dark and thus unable to come up with a better strategy to curb the rapid spread of coronavirus in Maharashtra, they said.
"I am told that out of 361 Covid-19 samples tested by the National Institute of Virology in Pune, 61 per cent had the double mutation. However, this sample size is too small to conclude as Maharashtra has been conducting nearly two lakh tests per day. One should not take such a small sample size as an indication that the mutated virus is widespread," a senior genome sequencing expert told PTI.
Maharashtra is witnessing an unprecedented spike in coronavirus positive cases for the last few weeks."
Source: https://timesofindia.indiatimes.com/city/mumbai/maharashtra-double-mutation-found-in-61-of-361-covid-19-samples-says-expert/articleshow/82066785.cms
Commentary: The strain afflicting this part of India, B.1.617, has two key mutations that allow for increased infectivity and better immune escape. That means the virus can spread faster and spread longer. Getting vaccines into large populations will be absolutely critical to prevent further, more effective mutations.
---
A reminder of the simple daily habits we should all be taking.
1. Always wear the best mask available to you when out of your home and you'll be around other people. Respirators are back in stock at online retailers, too. Wear an N95/FFP2/KN95 that's NIOSH-approved or better mask if you can obtain it. If you can't get an N95 mask, wear a surgical mask with a cloth mask over it.
2. Get vaccinated as soon as you're able to, and fulfill the full vaccine regimen.
3. Wash/sanitize your hands every time you are in or out of your home for any reason.
4. Stay home as much as possible. Minimize your contact with others and maintain physical distance of at LEAST 6 feet / 2 meters, preferably more. Avoid indoor places as much as you can; indoor spaces spread the disease through aerosols and distance is less effective at mitigating your risks.
5. Get your personal finances in order now. Cut all unnecessary costs.
6. Replenish your supplies as you use them. Avoid reducing your stores to pre-pandemic levels in case an outbreak causes unexpected supply chain disruptions.
7. Ventilate your home as frequently as weather and circumstances permit, except when you share close airspaces with other residences (like a window less than a meter away from a neighboring window).
8. Masks must fit properly to work. Here's how to properly fit a mask:
---
Common misinformation debunked!
There is no mercury or other heavy metals in the Pfizer mRNA vaccine. https://www.technologyreview.com/2020/12/09/1013538/what-are-the-ingredients-of-pfizers-covid-19-vaccine/
There is no genomic evidence at all that COVID-19 arrived before 2020 in the United States and therefore no hidden herd immunity:
Source:

There is no evidence SARS-CoV-2 was engineered, nor that it escaped a lab somewhere.
Source: https://www.washingtonpost.com/world/2020/01/29/experts-debunk-fringe-theory-linking-chinas-coronavirus-weapons-research/
Source: https://www.nature.com/articles/s41591-020-0820-9
Source: https://www.nationalgeographic.com/science/2020/05/anthony-fauci-no-scientific-evidence-the-coronavirus-was-made-in-a-chinese-lab-cvd/
There is no evidence a flu shot increases your COVID-19 risk.
Source: https://www.factcheck.org/2020/04/no-evidence-that-flu-shot-increases-risk-of-covid-19/
Source: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa626/5842161
---
A common request I'm asked is who I follow. Here's a public Twitter list of many of the sources I read.
https://twitter.com/i/lists/1260956929205112834
This list is biased by design. It is limited to authors who predominantly post in the English language. It is heavily biased towards individual researchers and away from institutions. It is biased towards those who publish or share research, data, papers, etc. I have made an attempt to follow researchers from different countries, and also to make the list reasonably gender-balanced, because multiple, diverse perspectives on research data are essential.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.