Lunchtime pandemic reading.
Standard disclaimer: this is a roundup of informative pieces I've read that interest me on the severity of the crisis and how to manage it. I am not a qualified medical expert in ANY sense; at best I am reasonably well-read laity. ALWAYS prioritize advice from qualified healthcare experts over some person on Facebook.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.
You are welcome to share this.
---
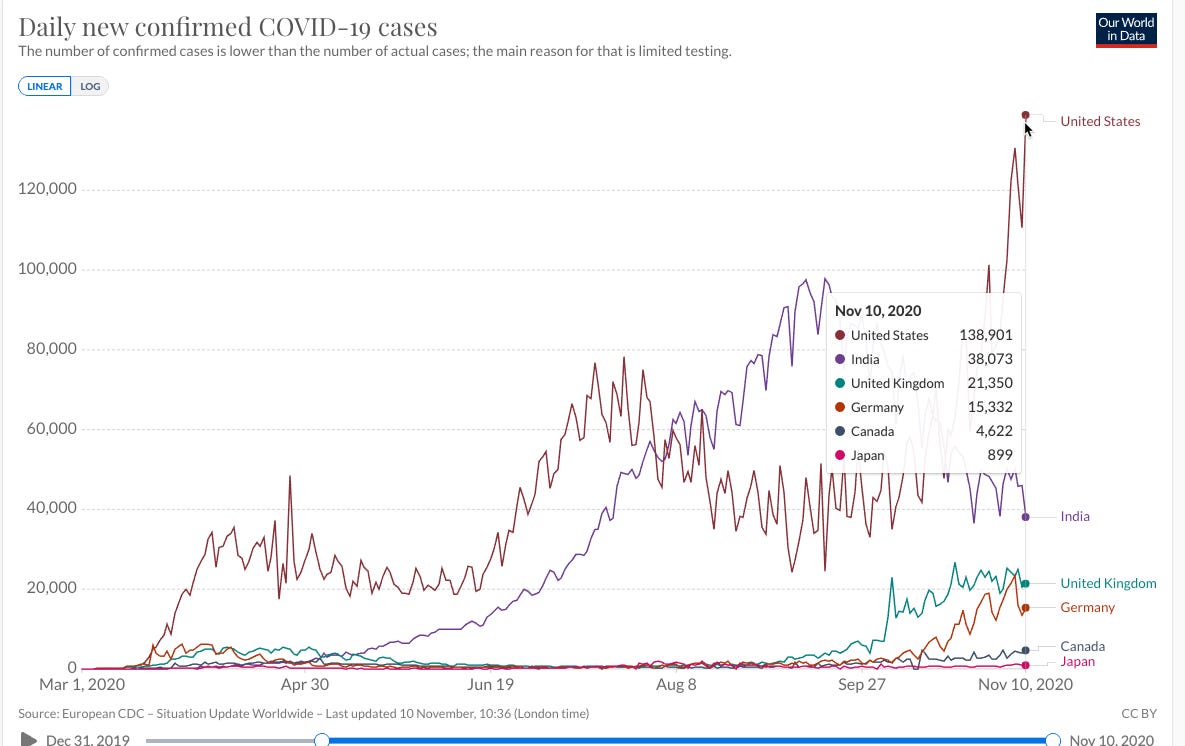
Planet-wide, we just crossed 500,000 new cases in a day. In America, where I live, we just hit an all-time record of 138,901 new cases in a day. Despite the excellent news about vaccine progress, at the moment things are worse, not better, and a vaccine that exists is not the same as a vaccine that has been distributed.
Stay safe.
---
More in-depth analysis on the Pfizer vaccine trial. "This alone is cause for celebration. Potentially. Many important questions remain unanswered. The first point that bears understanding is that "90% effective" means that many fewer test subjects who received the two-dose series of the real vaccine candidate developed symptomatic disease—the constellation of symptoms we call covid-19 disease. That does not necessarily mean that 90% fewer people became infected with the coronavirus itself. That's important because if a vaccinated person can still be infected, they might very well be able to pass along the disease to others who in turn may develop life-threatening covid-19, even if they themselves are at far lower risk of developing symptoms, let alone a bad or life-threatening case. Moreover, the fact that 90% fewer people who received the vaccine developed symptomatic disease could still end up being a kind of statistical mirage. We know that overall fewer than 1 percent of persons die as a result of being infected with SARS-CoV-2. If it turns out that those people are all among the 10% of the cases that still develop symptomatic disease despite vaccination, then today's results will have been highly disappointing in the final analysis. This isn;t to say that this is what happened. Rather, Pfizer released one piece of information—"datum" not "data." We are waiting and wanting more."
Source: https://brief19.com/2020/11/10/brief
Commentary: The key point here is we don't know yet from the trial whether or not the Pfizer vaccine stops spread, especially asymptomatic. That said, it's still amazing progress; the normal timeline for developing a vaccine is measured in years, not months.
---
COVID-19 has significant psychiatric side effects. "In patients with no previous psychiatric history, a diagnosis of COVID-19 was associated with increased incidence of a first psychiatric diagnosis in the following 14 to 90 days compared with six other health events (HR 2·1, 95% CI 1·8–2·5 vs influenza; 1·7, 1·5–1·9 vs other respiratory tract infections; 1·6, 1·4–1·9 vs skin infection; 1·6, 1·3–1·9 vs cholelithiasis; 2·2, 1·9–2·6 vs urolithiasis, and 2·1, 1·9–2·5 vs fracture of a large bone; all p<0·0001). The HR was greatest for anxiety disorders, insomnia, and dementia. We observed similar findings, although with smaller HRs, when relapses and new diagnoses were measured. The incidence of any psychiatric diagnosis in the 14 to 90 days after COVID-19 diagnosis was 18·1% (95% CI 17·6–18·6), including 5·8% (5·2–6·4) that were a first diagnosis. The incidence of a first diagnosis of dementia in the 14 to 90 days after COVID-19 diagnosis was 1·6% (95% CI 1·2–2·1) in people older than 65 years. A psychiatric diagnosis in the previous year was associated with a higher incidence of COVID-19 diagnosis (relative risk 1·65, 95% CI 1·59–1·71; p<0·0001). This risk was independent of known physical health risk factors for COVID-19, but we cannot exclude possible residual confounding by socioeconomic factors.
Survivors of COVID-19 appear to be at increased risk of psychiatric sequelae, and a psychiatric diagnosis might be an independent risk factor for COVID-19. Although preliminary, our findings have implications for clinical services, and prospective cohort studies are warranted.
Prospective cohort studies and longer-term follow-up studies are urgently needed to support and extend the findings of our study. Furthermore, enhanced psychiatric follow-up should be considered for patients who survive COVID-19. Finally, psychiatric history should be queried during assessment of a patient presenting with COVID-19 symptoms to adjust pre-test probability."
Source: https://www.thelancet.com/journals/lanpsy/article/PIIS2215-0366(20)30462-4/fulltext
Commentary: This is quite a serious complication; 18% - about 1 in 5 - survivors of COVID-19 develop a psychiatric diagnosis in this UK study. So let's recap for the COVID-19 deniers:
The infection fatality rate is about 0.97% - about a 1 in 100 chance overall of dying.
Long-haulers are anywhere from 5-20% of those who recover, having difficult, long recoveries.
And now 18% of people develop psychiatric issues of those who survive. That's quite frightening given how many tens or hundreds of thousands of people are being infected every day. This disease isn't going to kill en masse, but it sure is going to leave millions of people much worse off.
---
Face shields are ineffective alone. "Health care workers are exposed to potentially infectious airborne particles while providing routine care to coughing patients. However, much is not understood about the behavior of these aerosols and the risks they pose. We used a coughing patient simulator and a breathing worker simulator to investigate the exposure of health care workers to cough aerosol droplets, and to examine the efficacy of face shields in reducing this exposure. Our results showed that 0.9% of the initial burst of aerosol from a cough can be inhaled by a worker 46 cm (18 inches) from the patient. During testing of an influenza-laden cough aerosol with a volume median diameter (VMD) of 8.5 μm, wearing a face shield reduced the inhalational exposure of the worker by 96% in the period immediately after a cough. The face shield also reduced the surface contamination of a respirator by 97%. When a smaller cough aerosol was used (VMD = 3.4 μm), the face shield was less effective, blocking only 68% of the cough and 76% of the surface contamination. In the period from 1 to 30 minutes after a cough, during which the aerosol had dispersed throughout the room and larger particles had settled, the face shield reduced aerosol inhalation by only 23%. Increasing the distance between the patient and worker to 183 cm (72 inches) reduced the exposure to influenza that occurred immediately after a cough by 92%. Our results show that health care workers can inhale infectious airborne particles while treating a coughing patient. Face shields can substantially reduce the short-term exposure of health care workers to large infectious aerosol particles, but smaller particles can remain airborne longer and flow around the face shield more easily to be inhaled. Thus, face shields provide a useful adjunct to respiratory protection for workers caring for patients with respiratory infections. However, they cannot be used as a substitute for respiratory protection when it is needed."
Source: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4734356/
Commentary: This is no surprise. A disease that's an aerosol simply goes around a face shield. Remember the cigarette smoke test: would a face shield stop you from smelling someone else's cigarette smoke? Of course not. Nor will it stop you from inhaling their virus particles if they're infected.
---
Masks with valves need to have the valves covered in some fashion to offer protection to others. (they work fine for protecting you)
"This work demonstrates the qualitative fluid flow characteristics of a standard N95 respirator with and without an exhalation valve. Schlieren imaging was used to compare an adult male breathing through an N95 respirator with and without a valve. The schlieren imaging technique showed the flow of warm air passing through these respirators but did not provide information about droplet penetration. For this, strategic lighting of fog droplets was used with a mannequin head to visualize the penetration of droplets through both masks. The mannequin exhaled with a realistic flow rate and velocity that matched an adult male. The penetration of fog droplets was also visualized with a custom system that seals each respirator onto the end of a flow tube. Results of these qualitative experiments show that an N95 respirator without an exhalation valve is effective at blocking most droplets from penetrating through the mask material. Results also suggest that N95 respirators with exhalation valves are not appropriate as a source control strategy for reducing the proliferation of infectious diseases that spread via respiratory droplets."
Source: https://aip.scitation.org/doi/10.1063/5.0031996
Commentary: If you wear a mask with a valve, either modify it to filter the exhaust port or slap a simple mask on over top of it. That way, you're protecting others.
---
A reminder of the simple daily habits we should all be taking.
1. Wash/sanitize your hands every time you are in or out of your home for any reason. Consider also spraying the bottoms of your shoes with a general disinfectant (alcohol/bleach/peroxide) when you return home. Remember that cleaners are NEVER to be ingested or injected.
2. Always wear a mask when out of your home and if going to a high risk area, wear goggles. Respirators are back in stock at online retailers, too.
3. Stay home as much as possible. Minimize your contact with others and maintain physical distance of at LEAST 6 feet / 2 meters, preferably more. Avoid indoor places as much as you can; indoor spaces spread the disease through aerosols and distance is less effective at mitigating your risks.
4. Get your personal finances in order now. Cut all unnecessary costs.
5. Replenish your supplies as you use them. Avoid reducing your stores to pre-pandemic levels in case an outbreak causes unexpected supply chain disruptions.
6. Participate in your local political process. For Americans, go to Vote.org and register/verify your vote.
7. Ventilate your home as frequently as weather and circumstances permit.
---
Common misinformation debunked!
There is no genomic evidence at all that COVID-19 arrived before 2020 in the United States and therefore no hidden herd immunity:
Source:

There is no evidence SARS-CoV-2 was engineered, nor that it escaped a lab somewhere.
Source: https://www.washingtonpost.com/world/2020/01/29/experts-debunk-fringe-theory-linking-chinas-coronavirus-weapons-research/
Source: https://www.nature.com/articles/s41591-020-0820-9
Source: https://www.nationalgeographic.com/science/2020/05/anthony-fauci-no-scientific-evidence-the-coronavirus-was-made-in-a-chinese-lab-cvd/
There is no evidence a flu shot increases your COVID-19 risk.
Source: https://www.factcheck.org/2020/04/no-evidence-that-flu-shot-increases-risk-of-covid-19/
Source: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa626/5842161
---
A common request I'm asked is who I follow. Here's a public Twitter list of many of the sources I read.
https://twitter.com/i/lists/1260956929205112834
This list is biased by design. It is limited to authors who predominantly post in the English language. It is heavily biased towards individual researchers and away from institutions. It is biased towards those who publish or share research, data, papers, etc. I have made an attempt to follow researchers from different countries, and also to make the list reasonably gender-balanced, because multiple, diverse perspectives on research data are essential.
This is also available as an email newsletter at https://lunchtimepandemic.substack.com if you prefer the update in your inbox.